Exercise, Opioids, and the Cure for Chronic Pain
I’ve been thinking a lot about pain this week, mainly because I’ve been in a lot of it. In last week’s “Ode to my collarbone” I wrote about dealing with the immediate aftermath of a broken collarbone and briefly mentioned opioids, the very effective painkillers that can also carry a significant risk for abuse and addiction. Well, this weekend I’m back on those powerful painkillers following surgery to bolt my collarbone back together. However, my recent injury, research, and conversations with doctors and friends have led to an interesting conclusion about pain and painkillers:
For lifelong athletes, exercise can be both the cause and cure for chronic pain.
I have broken quite a few bones, and based on the comments, emails, and phone calls I’ve received, so have a lot of you! And even beyond broken bones, a lifetime of activity results in greater wear and tear on joints and more opportunities for ligament, tendon, and muscle injuries. Most of these injuries are relatively minor (thankfully) and only cause us to pause our active lifestyles for a little while. But in aggregate, over a period of 20-40 years, those acute injuries can add up to chronic pain.
A Brief History of Pain
Pain is remarkably difficult to measure. To make a comparison to athletic training, pain is essentially measured by perception, much like rating of perceived exertion (RPE). In sport we can correlate a subjective measure like RPE with objective data from power meters and heart rate monitors, but pain measurement is almost entirely subjective. And for a long time, physicians had effective ways to treat acute pain (anesthesia, nerve blocks, etc.) but far fewer options for treating chronic pain. As a result, people suffering from injuries or other painful conditions were often left debilitated, bedridden, unable to work or enjoy leisure time, and profoundly unhappy.
The emergence of prescription opioid painkillers like codeine, oxycodone, hydrocodone, and fentanyl provided physicians with highly effective medications for the pain management, and through both aggressive marketing and good intentions, the number of opioid prescriptions rapidly grew. People with debilitating pain experienced massive improvements in quality of life. They were able to complete activities of daily living with less pain or pain free. They were able to return to work, which was both fulfilling and lessened economic hardships. They were able to move more and be more active.
The addiction and overdose risks of opioids have been known for a long time. The prescription opioids you get from your doctor are not that far removed from heroin. And despite the fact the United States is in the midst of an opioid addiction and overdose crisis, the facts still remain that these medications are effective for pain management, most physicians prescribe them responsibly, and most patients take them as prescribed and stop taking them within a short period of time. And there are also doctors and patients using very powerful painkillers responsibly for long-term chronic pain, too. Personally, I am somewhat uneasy taking hydrocodone even for a few days, but Lord knows I’m grateful to have it this weekend!
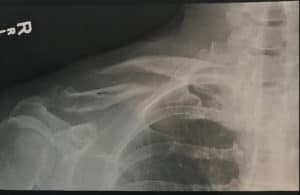
My collarbone, 8 days after my crash and not moving the right direction.

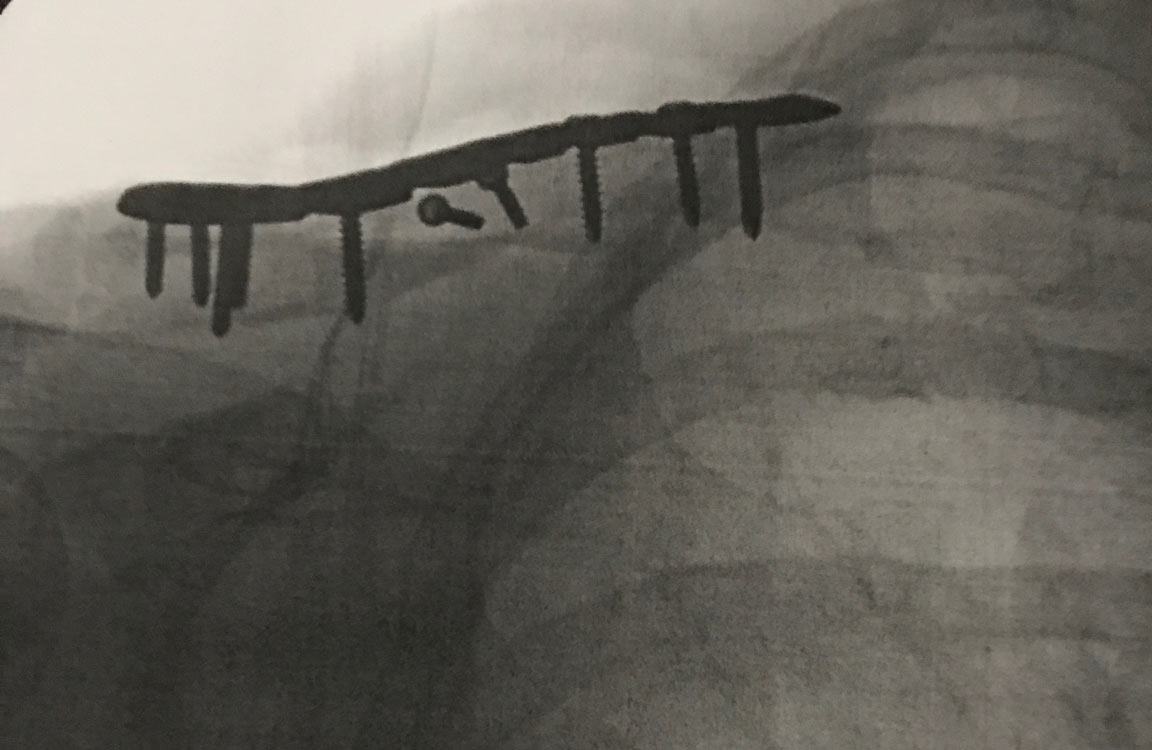
New hardware!
The Athlete’s Response to Pain
Athletes are not masochists, but I think we have a different relationship with pain compared to non-athletes. Training is strenuous. Discomfort is normal, and some level of pain is expected. We know injuries – both small and large – are part of the bargain. But athletes also learn early on that movement is part of the healing process.
Training is about taking proactive steps to improve performance. Pain limits our ability to perform, so we take steps to address pain through movement. At the simplest level, going for a light spin or walk on a recovery day is a means of alleviating pain from a prior effort. To address more significant pain we use physical therapy, massage therapy, compression garments and pneumatic boots, and a long list of other modalities.
► Free Cycling Training Assessment Quiz
Take our free 2-minute quiz to discover how effective your training is and get recommendations for how you can improve.
The medical establishment is catching on to this multi-modal approach to pain management. A report from National Public Radio describes “a biopsychosocial approach, [which] acknowledges not only the biological aspect of pain, but also recognizes that psychological and social variables contribute to how people experience pain.” The program at the Mayo Clinic seeks to help patients for whom pain medications are no longer effective, stating that opioid painkillers are neither recommended nor particularly effective for managing chronic pain. Instead of focusing on chemically blunting or blocking the pain, the focus is on regaining function so people can participate more fully in activities and relationships they find rewarding and valuable. The 40-year-old program has proven effective at getting many pain suffers off opioids by teaching participants to manage pain using multiple, non-pharmacological interventions.
Good Morale and Good Legs
When I was a young racer in Europe the old Belgian hard men used to say, “When the morale is good, the legs are good. When the legs are good, the morale is good.” As athletes, continuing to be active makes us feel good, and feeling good helps us stay active. My broken collarbone has been a good reminder that, while being an athlete has led to a number of injuries, being active has also kept chronic pain at bay.
In 1986 I broke my femur. It was a nasty break. I split the femoral condyle, messed up my patella, the works. To this day, my knee starts hurting any time I’m not active for an extended period of time. My good friend and NBA basketball legend, Bill Walton, is an even better (worse?) example. His career was cut short by repeated injuries to his feet, ankles, and spine. Standing and walking are painful for him every day. But put Bill on a bicycle and he’ll ride all day long. Next week he will ride down the coast of California, nearly 100 miles a day, during the Challenged Athlete Foundation Million Dollar Challenge (my recent crash is the only reason I’m not doing it with him). If you ask him he’ll tell you, “The bike is my gym, my wheelchair, and my church all in one.”
Without exercise, Bill Walton would be largely immobile. And while cycling is his form of exercise, in the larger picture it doesn’t have to be cycling. The point is that exercise keeps people moving, and moving keeps joints healthy. It keeps muscles, tendons, bones, and ligaments healthy. Exercise can prevent significant weight gain that leads to more joint pain and a host of other impediments to being active. And reduces cardiovascular disease risk as well as the risks of developing Type II Diabetes and hypertension. Perhaps most important – and a key point identified in the aforementioned Mayo Clinic program – is the psychological benefit being active imparts by enabling people to participate more fully in relationships, activities of daily life, and society in general.
An exercise program is not going to solve the nation’s opioid crisis or epidemic of chronic pain. But neither is the next narcotic painkiller. From where I (uncomfortably) sit, I believe it may be the culture of athletics – particularly the integration of exercise, diet, community, proactive recovery, and multi-modal therapies – that may provide the most promising model to inform and enhance the way the medical establishment tackles these public health crises.
Chris Carmichael
CEO/Head Coach of CTS
► FREE Mini-Course: Learn How to Maximize Your Limited Training Time
Learn step-by-step how to overcome limited training time and get faster. Walk away with a personalized plan to increase your performance.

Comments 30
Pingback: Managing Joint Pain Before Knee Replacement Surgery - Chris Carmichael
Pingback: For Pain Relief, the ‘a’ in CBDa Makes All the Difference - Chris Carmichael
Chronic pain: pain that persists more than 3 months in the course of repeated treatment is continuous. In case anybody thinks they know what it is. When you have gone thru this, then its given you a place at the table. Ive had 15 yrs of decent q of l but removal of medication is just cruel. There is no other treatment that requires compliance or forfiture of rights to decency, dignity and discrimination than pain treatment. Good luck of you break a leg or arm and you still have pain after a month. Suffer.
My pain is not due to phsyc probs. You get phsyc probs from unrelentingmpain due to the continued and inevitable deterioration of the body thru aging, use and injuries that all contribute. When the guy in line at the grocery store holds you up so he can meditate to releive his pain, what will you say to him?
I’m a 62 y/o F cyclist who started late in life. Just started having significant back pain that often keeps me from even washing dishes. Turns out I have severe stenosis of the spinal cord canal at L-4/L-5. It seems to be keeping me off the bike. Anyone out there have the same problem? How was it handled? I really want to road ride mountains and Colorado again.
–To the vet who is about to go through cancer treatment. Prayers to you. Keep charging on that bike. MP
16 years ago I was diagnosed with a similar condition, spondylolisthesis. At the spinal institute, they told me the surgery for my problem produced about 50% of the patients who said it was the best thing they’d ever done. The other 50% said it ruined their lives. The doctor advised me to put it off as long as possible, as there can always be better procedures discovered. They gave me a script for pain meds, & I was apprehensive. The doctor told me, “if I were a heart doctor & prescribed heart medication that would make your life better, would you want it?” I took the script & over the next several years, it was adjusted up & down to get to the exact spot where I could LIVE MY LIFE as close to normal as possible.
I’ve never attempted to get more medicine than what was prescribed, I’ve never had any “stolen,” I’ve never lost a whole bottle of pills, or tried to get them filled at multiple pharmacies. I get up every day & have a successful career. I have a family & am what most people would consider, a normal “contribute-to-society” individual. I exercise frequently, almost every day. I’m able to cycle & lift weights, do a bit of swimming & I thoroughly enjoy running. By exercising, I have been able to maintain the status of my spine rather than experience the deteriorating status which I was told is inevitable. (not to say it won’t happen, it hasn’t happened yet)
All this is due to the fact that I am able to take 4 pills within a 24 hour period that allow me the ability to sit at a desk, to drive to a gym, & to put on running shoes & exercise.
Now here we are in 2017 & I’m a criminal, an addict. A dredge to society.
Each quarter I check in with my doctor to ensure nothing has changed with my pain management. Last week when I saw him, I was given a pile of forms to fill out, & was told that from now on an office visit is required every month to fill my script, & I will be given random drug testing. If I am late for an appointment, my prescription will be terminated. That notice came along with 3 pages of brow-beating & discouraging verbiage. My health care just went up by the cost of an office visit x 12.
So this is where we are now as a society; we are no longer individuals with individual needs, problems, & solutions. If one of us is an addict, we all are.
Should the day come that I am no longer able to get the medication that allows me to live my life in the manner to which I am accustomed, I will no longer be able to work, exercise, or contribute to society. Those who are worried about the “opioid epidemic,” will be able to rest easy knowing they prevented another addict from ruining their life with drugs. Of course, they will be supporting my family financially, as I certainly won’t be able to. I’ll be nothing more than another disability statistic, but think of how good the do-gooders will feel!
THANK YOU! I am furious and miserable.The collective concience of the do gooders and power trippers,think what you said. I could add a bunch of obvious that you know. The climate is anbridled discrimination harrassment negative verbal conotations ,even profiling. A few stats for the perfect ones; <1%of pain patients died in 2016. There is NO other treatment in medical history,that FORCES compliance to recieve treatment. Under ADA these constitute discrimination,denial of right to treatment and a few others. Also,yes,there are other doctors,but theyre ALL doing this ,as per discrimination. As this is happening to vets,cancer patients ,chronic pain and seniors. There is clear mental and verbal abuse aimed at all these groups at doctors offices by all from doctors,office staff nurses and especially profiling at pharmacies. Numerous stories, one CVS pharmacy teach of 30yrs said,for example,anyone with visible tatoos were automaticly denied meds. Also,they were told to lie and say theyre out of certain opioid meds based on a patient being unshaven,looked dischevled(im barely able to "pretty myself) are denied meds. Im concerned for all the addicts,i have a heart. But opioids are opium,opium is heroin. Opium has 3k of history of addictive prop and doctors claim they got duped by a sales pitch? There is laughable "wasnt me" to the statment. Drs spend 10+ yrs in school dont tell me they didnt know the history or connection. I learned in 7th grade in the early 80s. This side point. But today, being a 15yr chronic pain patient,my meds cut off in august 2017, im barely able to get to or use the toilet. The alt medicine of yoga acupuncture exercise meditation are infantile and inneffective . With the exsisting deterioration and continued deterioration of my body. These treatments are limited to barely 6hrs if im lucky. So im supposed to meditate when my pain hits,say behind the wheel? Grocery store? Or late to a dr appt becausemi needed to do an hour of yoga to get a distinctly limited hour or two of reduced pain ? Please, spare me. None of these therapies is certified or backed by data and stats, as the only stats about my meds is, presented negatively. Hundreds of thousands of positive, improved quality life stories on the web, facebook and twitter. Forrest Tennant is the authority on prescribing for chronic pain. Never once have christie or gotlieb,or the socalled experts presented his,positive competent guidelines. CDC FDA DEA are all touting stats and studies that its been proven, are skewed and innacurate in thier assumptions
Thats more than i have in me to write so im done. Gona go suffer, cry and contemplate suicide now. Cause this situation is killing me. Thank you
Training for life itself! Godspeed Chris in your recovery.
Pingback: Ultramarathon Daily News | Monday, Oct 16 | Ultrarunnerpodcast
I pray for your quick healing. I broke my collar bone a couple of years back and after a talk with the orthopedist I decide to just tolerate it. My break was very annoying until I started working out on a great exercise program and this helped strengthen the shoulder, return range of motion and strength. sure I still feel it but there is no pain. I also would suggest a good multi-mineral supplement. this really fights degenerative bone diseases. Thanks for your timely advice.
Just a warning – I had pre-planned back fusion surgery last month (L3-4) (2 days after participating in Rebecca Rusch’s excellent gravel grinder). I was prescribed oxycodone for pain management, told by multiple nurses to stay ahead of the pain and take a muscle relaxer to supplement the Oxy. I was in the hospital one night post-op, at home for 2 days taking the prescribed and same dosages of the Oxy and muscle relaxer that I was given in the hospital, all on a full stomach. I overdosed. Over the next 24 hours 3 physicians (including the ER doc) told me I would have died if my girlfriend hadn’t, by chance, checked in on me – where she found me purple and not breathing. She was unable to wake me up and immediately called 911. Be very very careful with Opioid dosages (EVEN PRESCRIBED DOSAGES!!), do not combine with a muscle relaxer unless absolutely necessary for pain management and don’t take the opioids if you can avoid them. After my additional night in the hospital following the OD, I stopped taking the stuff, thankful to have survived – and looking forward to riding again early next spring after my fusion takes.
Chris,
7 years ago my x-rays looked exactly like yours. Yes, the surgery does work wonderfully and quickly. Just want you to remind you, even as we age, just how resilient the human body is. I would add yoga to the list of alternative means of keeping pain away. It’s an everyday habit for me. I hope you are back out there soon and feeling 100%.
P.S. As a 63 year old female, I don’t do single-track any more:)
I agree – but you are preaching to the choir 🙂
Broken many bones mostly downhilling or gravity as they call it. Just part of the sport. Never done the opioids over a day. Makes you too slow and doppy. Who would want that? The sooner you are active the better. I can recall several times ridding while still in a cast. Opioids? As little as possible or none.
Enjoyed the article about a very common problem. In spite of medical and surgical advances back pain in particular continues to be an enigma for patients who suffer. One common mistake is rushing into surgery before exhaustingbither options, e.g., PT, massage, low-impact exercise and stretching. Although NSAIDS are very helpful for many are not aware that they are not recommended for chronic use due to the risk of heart attacks and stoke. FDA has even strengthened its initial warning. One should discuss this with their doctor.
Hi Chris, having never broken a bone in my body, I have no reference to compare, but I have had serious physical pain and it is how we deal with it that is key. I’m so glad that you have a grown up attitude to opioids and that you have highlighted the dangers of over reliance on pain killers. I am not an athlete with miles on the clock that you clearly have, but I hope to be one day, hopefully without the scars! Thanks and hoping you have a quick recovery.
I had a bike accident in July lost two unit of blood and in Critical Care Unit for four days. No broken bones this time, but muscles Seriously damaged. The pain from broken bones and damaged muscles I am can handle. I got shingles two weeks after my accident , which is total different because it nerve pain and nothing seems to work . I missed hill climbing camp in Brevard , be back next year. I am 74 and was in the best ship om life when I the accident.
barry
I am presently 2 weeks out from a gravel grinder accident that I can not remember due to a head injury. In addition to what is being called a concussion I sustained a fractured pelvis and perhaps an injury not yet diagnosed to my once repaired right shoulder. I have additional contusions that are also quite painful. At first I cringed at the thought of taking narcotic pain medication. Two weeks out I am still quite debilitated and have decided that I can not longer withstand the constant pain. I have decided to take the minimally prescribed dose of pain medication. This has resulted in better rest and slightly better movement which by my medical background means both a better physical and mental recovery. I plan on returning to my prior addiction, cycling. Thank you for this forum.
Great article (as ever) and wishing you a speedy recovery Chris.
There is also another often overlooked and dismissed way of thinking about pain which examines the psychological basis of it. I’m not talking about a broken collar bone or femur – clearly this pain has a structural cause. However, many people experience chronic pain seemingly without a structural reason (back pain probably being the most common) and for many others the structural ‘reason’ may not really be the cause. MRIs scans of healthy adults who have never experienced back pain show ruptured and bulging discs for example. My own journey of dealing with back pain through repeated ‘physical’ interventions was without progress until I discovered the psychological approach – this was the only thing that actually helped. And, to be clear I’m absolutely not suggestion that all pain has a psychological component, I broke my femur a couple of years ago, I’m aware of what that is like. This line of enquiry into pain will be difficult for many people and in Western society we locked into a structural cause-effect paradigm. I’m not posting this to argue with anyone, if you think it’s a load of rubbish i understand but I post for those who might want to know more and for whom it might help. John Sarno’s ‘The MindBody Prescription’ book is a good starting point.
6 days until you are on the wind trainer, 2 weeks until you are hiking the Garden of the Gods, 4 weeks until riding the neighborhood, 6 weeks back on the Chutes.
12 weeks get the hardware out!
Heal Strong.
Great article.
TENS. Is also a great adjunct for acute, chronic and post operative pain management. It is relatively inexpensive and can provide major benefits to assist in relieving pain and resetting the “sensitivity/hyperactivity ” that can occur in the nerves.
Get well soon!
Great article, I have been dealing with chronic pain for over 25 years due to a knee injury. I have been on Opioids for as long as they have been out. Got back in to cycling 3 years ago after trying rest and many other option.
Being back on the bike has been great.
It helps with building the muscles back but the riding helps clear my mind. I am working on getting off the Opioids but have to do it over time due to the length of time I have been on them.
Great article. I am 79 years old and try to ride at least 100 miles per week. I have several physical problems but the most difficult is arthritis in my hands. I get out there and just keep on going. I know if I stop I probably will just wither up and die. Your advice is well taken. Thank you.
Thanks for posting. What a role model. Modest but an achiever, no doubt. I’m a couple of decades behind, but if I can do 100 miles on the bike at 4 score, I’ll be a very happy “bunny”. Cheers
Ice.
I’m 81, collar bone, shoulder, knees, ribs, have all been broken. Ice it until you can’t feel it, wait until it hurts and ice it again.
Great article, thank you for sharing. Good Morale Good Legs! Heal up soon.
Motion is lotion is a term I learned form a very wise physical therapy professor 25 years ago in school. I too have had many injuries and multiple knee surgeries and the bike is the best modality for my chronic pain. I have converted so many runners to cyclists over the year that I have stopped counting, since it is so much friendlier to the joints.
This really hits home. I am dealing with chronic pain from my military service injury and on top of that bone cancer. I have been prescribed painkillers that make hydrocodone look like ibuprofen. I avoid taking it as much as possible and I use Cycling and biofeedback to bring the pain done to a tolerable level. I am never out of pain , but a good long ride with lots of climbing and a little friendly competition amongst Cycling brothers and sisters seem to help me put the pain out of mind. Great article and so relevant as I leave for the United Healthcare /ProjectHero/Ride2Recovery California Challenge 7 day ride. When I return I will be undergoing cancer surgery that will keep me from riding outside for a few months. I hope as soon as I can swing my legs over my bike on a trainer ; I will be riding that until I can hit the road.
Good insights and well said.
If you don’t stop moving, you won’t get stuck. Get well soon.